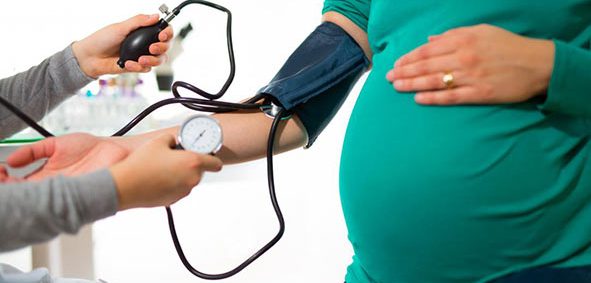
Pre-Eclampsia
Pre-eclampsia is a condition all pregnant mums should be aware of, so you can monitor yourself for symptoms and ensure you get help as soon as you need it.
What is pre-eclampsia?
Pre-eclampsia is a serious condition involving high blood pressure and high protein levels in your urine, and it can have dangerous effects on your other body organs as well as be harmful to your developing baby. It typically happens after the 20th week of pregnancy and can last for two or three weeks following your baby’s birth. Pre-eclampsia occurs in about 8% of pregnancies, and accounts for about 15% of premature births. It needs to be diagnosed and treated by a medical professional such as your LMC or GP. If you think you have any of the symptoms of pre-eclampsia, don’t hesitate. Get in touch with your LMC straightaway.
What are the signs and symptoms of pre-eclampsia?
Pre-eclampsia can develop without symptoms that you notice, which is why it’s important to go to your LMC appointments every time. Here are some of the symptoms you might notice if they do develop:
- A severe headache that won’t go away
- Seeing spots or flashes of light
- Blurry vision
- Sudden swelling in your ankles, legs, feet, face, hands, or eyes – remember that some swelling in normal during pregnancy, but if it comes on quickly, this can be a sign
- Sudden weight gain – more than 1kg in a week
- Pain in your upper stomach or shoulder
- Shortness of breath and difficulty breathing
- Vomiting after 20 weeks of pregnancy (not to be confused with hyperemesis gravidarum, which is severe morning sickness and should generally be diagnosed early in pregnancy)
How do I know if I’m at risk of developing pre-eclampsia?
While the medical field still hasn’t figured out exactly what causes pre-eclampsia, they have identified some risk factors that seem to correlate with a higher chance of developing pre-eclampsia. You have a higher chance of developing pre-eclampsia if:
- You are a first-time mum
- It has been more than 10 years since you had your last baby
- You have a sister or mother who also had pre-eclampsia
- You have had pre-eclampsia in a previous pregnancy
- You are over the age of 40
- You are expecting multiple babies (twins, triplets etc)
- You are overweight
- You already had high blood pressure (hypertension) before you got pregnant
- You have kidney disease or diabetes
- You had low levels of placental hormones in your first trimester
- You had IVF
This is not an exhaustive list; there are other more rare risk factors, but your midwife should screen you for these when you have your antenatal appointments.
How is pre-eclampsia treated?
Because pre-eclampsia is a condition of pregnancy, it won’t go away until your baby is born, and can linger for a few weeks following your baby’s birth. If you are diagnosed with pre-eclampsia or if your LMC or midwife is concerned, you will be referred to an obstetrician or specialist, and they will see you pretty quickly. Your LMC or specialist will arrange for further tests, and you may need to be admitted to hospital or put on bed rest until your baby is born.
You may be given medication to lower your blood pressure, and will possibly be advised to decrease your activity levels, avoid stress and anxiety, and rest your body. You may need to stop working.
If your pre-eclampsia is diagnosed near the end of your pregnancy, your LMC or specialist may recommend inducing labour and delivering your baby early.
If you are not at the end of your pregnancy but your LMC or specialist is concerned about pre-eclampsia having detrimental effects on your baby, your baby may need to be delivered pre-term. This is a situation your LMC or specialist will discuss with you, and you may need other medications or treatment in order to give your baby the best chance possible of being healthy.
How worried should I really be?
Pre-eclampsia is a serious condition, but modern maternity care gives you a good chance of having it diagnosed and treated in time. Most of the women who have the conditions described in the symptom list above do not develop pre-eclampsia. However, you still need to have your blood pressure and urine checked at each antenatal visit, and listen to your LMC or midwife if she wants you to monitor certain symptoms or change your activity levels.
With pregnancy, usually “better safe than sorry” is a good rule to follow. If something feels “off” or you start to notice any of the symptoms above, get in touch with your LMC and arrange for a checkup. Don’t worry that you’re being a bother or overreacting – you know your own body, and you have your baby’s best interests at heart. If your mental health is affected by anything you are experiencing in pregnancy, or if you find yourself worrying too much and getting very anxious, talk to your LMC about this as they can help you access maternal mental health support.
– You may also like –
 |
 |
 |